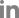ŽÖľ žĚė
Ž≥ł žóįÍĶ¨ŽäĒ žĚľ žÉĀͳȞĘÖŪē©Ž≥ĎžõźžóźžĄú žąúŪôė 3ÍĶźŽĆÄÍ∑ľŽ¨īŽ•ľ ŪēėÍ≥† žěąŽäĒ ÍįĄŪėłžā¨Ž•ľ ŽĆÄžÉĀžúľŽ°ú žĚľž£ľÍłįžú†Ūėēžóź ŽĒįŽĚľ Í∑ľŽ¨īž°įŽ≥Ą žąėŽ©īžčúÍįĄÍ≥ľ žā¨ŪöĆž†Ā žčúžį®Ž•ľ ŪôēžĚłŪēėÍ≥†, ž£ľÍīÄž†ĀžúľŽ°ú žĚłžčĚŪēėŽäĒ žąėŽ©īžě•žē†Ž•ľ ž°įžā¨Ūēėžó¨ ŪĖ•ŪõĄ ÍįĄŪėłžā¨žĚė ÍĶźŽĆÄÍ∑ľŽ¨īžóź ŽĆÄŪēú Žįúž†Ąž†Ā ŽĆÄžēąžĚĄ žąėŽ¶ĹŪēėŽäĒŽćį ÍłįžīąžěźŽ£ĆŽ°ú Ūôúžö©ŪēėÍ≥†žěź žąėŪĖČŽźėžóąÍ≥†, Í≤įÍ≥ľžóź ÍłįŽįėŪēėžó¨ ŽÖľžĚėŽ•ľ žßĄŪĖČŪēėÍ≥†žěź ŪēúŽč§.
Ž≥ł žóįÍĶ¨ ŽĆÄžÉĀžěźžĚė žĚľž£ľÍłįžú†ŪėēŽ≥Ą Í∑ľŽ¨īž°įŽ≥Ą žąėŽ©īžčúÍįĄžĚĄ ž°įžā¨Ūēú Í≤įÍ≥ľ, Í∑ľŽ¨īžĚľžĚė Í≤Ĺžöį ŽāģŽ≤ąžĚÄ ž†ÄŽÖĀŪėēÍĶįžóźžĄú, žīąŽ≤ąžĚÄ žēĄžĻ®ŪėēÍĶįžóźžĄú ŪŹČÍ∑† žąėŽ©īžčúÍįĄžĚī ÍįÄžě• žßßžēėÍ≥†, Žį§Ž≤ąžĚÄ žĚľž£ľÍłįžú†Ūėēžóź ŽĒįŽ•ł žį®žĚīŽäĒ žóÜžóąŽč§. ŽėźŪēú žĚľž£ľÍłįžú†ŪėēŽ≥Ą Í∑ľŽ¨īžĚľžĚė žąėŽ©īžčúÍįĄ Í≤©žį®ÍįÄ ÍįÄžě• ŪĀį Í∑ľŽ¨īž°įŽäĒ žīąŽ≤ąžúľŽ°ú 2žčúÍįĄ žĚīžÉĀ žį®žĚīŽ•ľ Ž≥īžėÄŽč§. žĚīŽ†áÍ≤Ć žĚľž£ľÍłįžú†ŪėēŽ≥Ą Í∑ľŽ¨īž°įŽßąŽč§ žąėŽ©īžčúÍįĄžĚī Žč§Ž•ł žĄĪŪĖ•žĚĄ Ž≥īžĚīŽäĒ Í≤ÉžĚÄ 3ÍĶźŽĆÄÍ∑ľŽ¨ī Í≤ĹžįįŽď§(32.1¬Ī5.4žĄł)žĚĄ ŽĆÄžÉĀžúľŽ°ú Ūēú žļźŽāėŽč§žĚė žóįÍĶ¨[
24]žôÄ žú†žā¨ŪēėžėÄŽč§. Ž≥ł žóįÍĶ¨ ŽĆÄžÉĀžěźžĚė ŽāģŽ≤ąÍ≥ľ Žį§Ž≤ą Í∑ľŽ¨īžĚľžĚė žąėŽ©īžčúÍįĄžĚÄ 4.68-5.90žčúÍįĄžúľŽ°ú, žļźŽāėŽč§ 6Íįú Ž≥ĎžõźžĚė ÍĶźŽĆÄÍ∑ľŽ¨īžěź(89%ÍįÄ ÍįĄŪėłžā¨, 38.72¬Ī11.08žĄł)žôÄ ž£ľÍįĄ žÉĀÍ∑ľžěź(44.92¬Ī10.04žĄł)Ž•ľ ŽĆÄžÉĀžúľŽ°ú Í∑ľŽ¨īžĚľžĚė žąėŽ©īžčúÍįĄžĚĄ ž°įžā¨Ūēú žóįÍĶ¨[
25]žóźžĄú ÍĶźŽĆÄÍ∑ľŽ¨īžěźžĚė Í∑ľŽ¨īžĚľ ŪŹČÍ∑† žąėŽ©īžčúÍįĄžĚī 5.53žčúÍįĄžĚīŽĚľÍ≥† Ž≥īÍ≥†Ūēú Í≤įÍ≥ľžôÄ žú†žā¨ŪēúŽćį, žĚī žóįÍĶ¨žóźžĄú žÉĀÍ∑ľžěźžĚė Í∑ľŽ¨īžĚľ žąėŽ©īžčúÍįĄžĚī 6.72žčúÍįĄžĚł Í≤Éžóź ŽĻĄŪēėŽ©ī ÍĶźŽĆÄÍ∑ľŽ¨īžěźžĚė Í∑ľŽ¨īžĚľ žąėŽ©īžčúÍįĄžĚī Ūēú žčúÍįĄ žĚīžÉĀ žßßžēėŽč§. žú†ŽüŞ󟞥ú 65,000Ž™Ö žĚīžÉĀžĚī žįłžó¨Ūēú ŽĆÄÍ∑úŽ™® žĚłÍĶ¨ž°įžā¨ žóįÍĶ¨[
26]žóźžĄú 20ŽĆÄŽ∂ÄŪĄįŽäĒ žóįŽ†ĻžĚī ž¶ĚÍįÄŪē†žąėŽ°Ě Í∑ľŽ¨īžĚľÍ≥ľ ŪúīžĚľ Ž™®ŽĎźžóźžĄú žąėŽ©īžčúÍįĄžĚī ž§ĄžĖīŽď§Í≥†, žó¨žĄĪŽ≥īŽč§ Žā®žĄĪžĚė žąėŽ©īžčúÍįĄžĚī ŽćĒ žßߎč§Í≥† Ž≥īÍ≥†Ūēú Í≤ɞ̥ Í≥†Ž†§ŪēúŽč§Ž©ī, ÍĶźŽĆÄÍ∑ľŽ¨īžěźžĚė žąėŽ©īžčúÍįĄžĚī žÉĀÍ∑ľžěźžóź ŽĻĄŪēī ŪėĄž†ÄŪěą ž†ĀÍ≥†, ŪäĻŪěą Ž≥ł žóįÍĶ¨ ŽĆÄžÉĀ ÍįĄŪėłžā¨Žď§žĚī žĄ†ŪĖČžóįÍĶ¨ ŽĆÄžÉĀžěźŽď§Ž≥īŽč§ ŽćĒ žóįŽ†ĻžĚī ž†ĀÍ≥† ŽĆÄŽ∂ÄŽ∂Ą žó¨žĄĪžěĄžóźŽŹĄ Ž∂ąÍĶ¨ŪēėÍ≥† žąėŽ©īžčúÍįĄžĚī ŽćĒ žßßžĚÄ Í≤ÉžúľŽ°ú ŽāėŪÉÄŽā¨Žč§. ÍĶźŽĆÄÍ∑ľŽ¨īžěźŽäĒ ž†ēžÉĀž†ĀžĚł žąėŽ©ī-ÍįĀžĄĪ ž£ľÍłįŽ•ľ Ž≤óžĖīŽāú žčúÍįĄŽĆÄžóź žąėŽ©īžĚĄ ž∑®ŪēėÍłį ŽēĆŽ¨łžóź žąėŽ©īžĚė žßąžĚī ŽĖ®žĖīžßÄÍ≥† žąėŽ©ī žú†žßÄžóź žĖīŽ†§žõÄžĚī žěąžĖī[
4] žąėŽ©īžčúÍįĄžĚī žßßžēĄž°ĆžĚĄ Í≤ÉžúľŽ°ú žÉĚÍįĀŽźúŽč§.
ŪēúŪéł, ÍįĚÍīÄž†Ā žąėŽ©īžł°ž†ēŽŹĄÍĶ¨žĚł žē°ŪčįÍ∑łŽěėŪĒĄŽ•ľ žĚīžö©Ūēī ÍĶźŽĆÄÍ∑ľŽ¨īÍįĄŪėłžā¨Žď§žĚė žąėŽ©īžĚĄ žł°ž†ēŪēú ŽĎź ŪéłžĚė ÍĶ≠ŽāīžóįÍĶ¨žóźžĄú Í∑ľŽ¨īž°įŽ≥Ą Í∑ľŽ¨īžĚľžĚė žąėŽ©īžčúÍįĄžĚÄ ŽāģŽ≤ąžĚÄ Ž≥ł žóįÍĶ¨žôÄ žú†žā¨ŪēėÍ≤Ć Ž™®ŽĎź 6žčúÍįĄ ŽĮłŽßĆžúľŽ°ú ŽĻĄžä∑ŪēėŽāė, Žį§Ž≤ą Í∑ľŽ¨īžĚľžĚė žąėŽ©īžčúÍįĄžĚÄ 7.18žčúÍįĄ[
16]Í≥ľ 6.07žčúÍįĄ[
17]žúľŽ°ú žóįÍĶ¨ŽßąŽč§ žį®žĚīŽ•ľ Ž≥īžėÄžúľŽ©į, Ž≥ł žóįÍĶ¨ ŽĆÄžÉĀžěźžĚė ž£ľÍīÄž†Ā žąėŽ©īžčúÍįĄžĚł 5.40-5.90žčúÍįĄŽ≥īŽč§ ŽćĒ Íłī Í≤ÉžúľŽ°ú ŽāėŪÉÄŽā¨Žč§. žē°ŪčįÍ∑łŽěėŪĒĄŽ°ú žł°ž†ēŪēú žĄ†ŪĖČžóįÍĶ¨žĚė ŽĆÄžÉĀžěź žąėÍįÄ Ž™®ŽĎź 20Ž™Ö ŽĮłŽßĆžúľŽ°ú ž†ĀžĖīžĄú, ÍįĚÍīÄž†Ā žąėŽ©īžčúÍįĄÍ≥ľ ž£ľÍīÄž†Ā žąėŽ©īžčúÍįĄžĚė žį®žĚīŽ•ľ žĄ§Ž™ÖŪēėÍłį žúĄŪēīžĄúŽäĒ žĘÄ ŽćĒ ŽßéžĚÄ žąėŽ•ľ ŽĆÄžÉĀžúľŽ°ú Ūēú ŽįėŽ≥ĶžóįÍĶ¨ŽŹĄ ŪēĄžöĒŪēėÍ≤†Žč§.
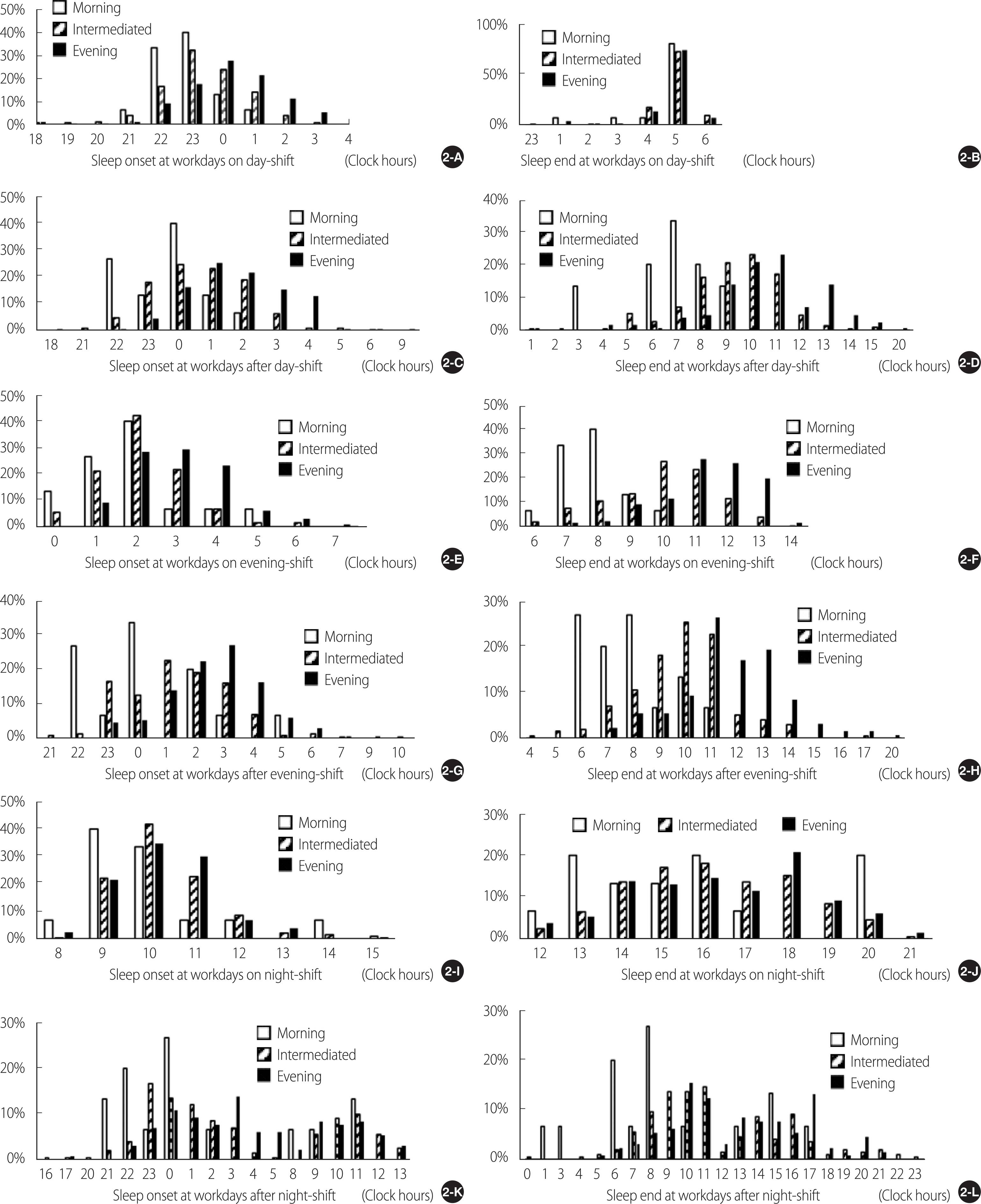
Í∑ľŽ¨īž°įŽ≥Ą žąėŽ©ī žčúžěĎ žčúÍįĀÍ≥ľ žąėŽ©īžĚī ŽĀĚŽāėŽäĒ žčúÍįĀžĚĄ žāīŪéīŽ≥īŽ©ī, ŽāģŽ≤ą Í∑ľŽ¨īžĚľžóź žąėŽ©īžĚī ŽĀĚŽāėŽäĒ žčúÍįĀžĚī ž∂úÍ∑ľžčúÍįĄ ŽēĆŽ¨łžóź Ž™®Žď† žĚľž£ľÍłįžú†ŪėēžóźžĄú 5žčúŽĆÄžóź žßĎž§ĎŽźėžĖī Ž∂ĄŪŹ¨ŽźėžĖī žěąžúľŽāė, ž†ÄŽÖĀŪėēÍĶįžĚė Í≤Ĺžöį žąėŽ©ī žčúžěĎ žčúÍįĀžĚī 0žčú žĚīŪõĄžĚł ŽĆÄžÉĀžěźÍįÄ ŽćĒ ŽßéžēĄžĄú žąėŽ©īžčúÍįĄžĚī žßßžĚÄ Í≤ÉžúľŽ°ú ŽāėŪÉÄŽā¨Žč§. ŽāģŽ≤ą Í∑ľŽ¨īžĚľžĚė žąėŽ©īžčúÍįĄžĚī žßßžĚÄ ž†ÄŽÖĀŪėēÍĶįžĚÄ ŽāģŽ≤ą ŪõĄ ŪúīžĚľžĚė žąėŽ©īžčúÍįĄžĚī ÍįÄžě• ÍłłžĖīžĄú Í∑ľŽ¨īžĚľÍ≥ľ ŪúīžĚľ ÍįĄ žā¨ŪöĆž†Ā žčúžį®ÍįÄ 3.87žčúÍįĄžúľŽ°ú ÍįÄžě• ŪĀį žčúžį®Ž•ľ Ž≥īžėÄŽč§. žĚīŽäĒ ÍĶźŽĆÄÍ∑ľŽ¨īÍįÄ ŽāģŽ≤ąžĚł Í≤Ĺžöį žĚľž£ľÍłįžú†ŪėēžĚī ž†ÄŽÖĀŪėēžĚľžąėŽ°Ě žąėŽ©īžčúÍįĄžĚī žßßžĚÄ Í≤ÉžúľŽ°ú Ž≥īÍ≥†Ūēú žĄ†ŪĖČžóįÍĶ¨[
11]žôÄ žĚľžĻėŪēėŽäĒ Í≤įÍ≥ľžĚīŽč§. žĚīŽäĒ ŽāģŽ≤ą Í∑ľŽ¨īŽäĒ ž∂úÍ∑ľžčúÍįĄ ŽēĆŽ¨łžóź žąėŽ©īžĚī ŽĀĚŽāėŽäĒ žčúÍįĀžĚī ž†ēŪēīž†ł žěąžßÄŽßĆ, žąėŽ©ī žčúžěĎ žčúÍįĀžĚÄ žĚľž£ľÍłįžú†ŪėēžĚė žėĀŪĖ•žĚī žĽ§žĄú ž†ÄŽÖĀŪėēÍĶįžĚÄ žĚľžįć žě†Žď§žßÄ Ž™ĽŪēėÍłį ŽēĆŽ¨łžúľŽ°ú ž∂Ēž†ēŽźúŽč§. van de Ven ŽďĪ[
27]žĚė žóįÍĶ¨žóźžĄú žĚľž£ľÍłįžú†ŪėēžĚī ž†ÄŽÖĀŪėēžĚł žßώ讞󟞥ú ÍłįžÉĀžčúÍįĄžĚī žěźžú†Ž°úžöī žīąŽ≤ą Í∑ľŽ¨īžóź ŽĻĄŪēī ŽāģŽ≤ą Í∑ľŽ¨ī žčú žě†ÍĻ®ÍłįÍįÄ žĖīŽ†ĶÍ≥†(difficulties waking up), ŪöĆŽ≥ĶŽźėžßÄ žēäŽäĒ žąėŽ©ī(non-refreshing sleep)Í≥ľ ÍłįžÉĀ žčú ŪĒľÍ≥§Ūē®(exhausted at awakening)žĚĄ ŽāėŪÉÄŽāīŽäĒ ÍįĀžĄĪŽ∂ąŽßĆžßÄžąė(awakening complaint index)ÍįÄ ŽÜíŽč§Í≥† ŪēėžėÄŽč§. ŽĒįŽĚľžĄú ž†ÄŽÖĀŪėē žĚľž£ľÍłįžú†ŪėēžĚĄ ÍįĞߥ žā¨ŽěƎ吏óźÍ≤ĆŽäĒ ÍįÄŽä•ŪēėŽ©ī ŽāģŽ≤ą Í∑ľŽ¨ī ŽįįžĻėŽ•ľ ž§Ąžó¨ž§Ą ŪēĄžöĒÍįÄ žěąŽč§. Í≥Ķžě•Í∑ľŽ°úžěźŽ•ľ ŽĆÄžÉĀžúľŽ°ú žĚľž£ľÍłįžú†ŪėēžĚī ž†ÄŽÖĀŪėēžĚł Í≤Ĺžöį ŽāģŽ≤ą Í∑ľŽ¨īŽ•ľ ž§ĄžĚīÍ≥†, žēĄžĻ®ŪėēžĚł Í≤Ĺžöį ŽāģŽ≤ą Í∑ľŽ¨īŽ•ľ ŽäėŽ¶¨Í≥† Žį§Ž≤ą Í∑ľŽ¨īŽ•ľ ž†ĀÍ≤Ć ŽįįžĻėŪēėžěź ž£ľÍīÄž†Ā žąėŽ©īžĚė žßąžĚī žÉĀžäĻŪēėÍ≥†, Í∑ľŽ¨īžĚľžĚė žąėŽ©īžčúÍįĄžĚī ŪŹČÍ∑† 30Ž∂Ą žĚīžÉĀ ŽäėžĖīŽā¨žúľŽ©į, žā¨ŪöĆž†Ā žčúžį®ŽŹĄ 1žčúÍįĄ žĚīžÉĀ ÍįźžÜĆŪĖąŽč§Í≥† Ž≥īÍ≥†Ūēú žóįÍĶ¨[
28]Ž•ľ Í≥†Ž†§ŪĖąžĚĄ ŽēĆ ŽāģŽ≤ą, žīąŽ≤ą, Žį§Ž≤ą Í∑ľŽ¨īÍįÄ Ž™®ŽĎź ŽįįžĻėŽźėŽäĒ ž†ĄŪėēž†ĀžĚł 3ÍĶźŽĆÄ Žį©žčĚŽ≥īŽč§ŽäĒ ÍįúžĚłžĚė žĚľž£ľÍłįžú†Ūėēžóź Žßěž∂į ž†ĀžĚĎžĚī žĖīŽ†§žöī Í∑ľŽ¨īž°įŽ•ľ ŽļÄ 8žčúÍįĄ 2ÍĶźŽĆÄ(žėą. ŽāģŽ≤ą-žīąŽ≤ą, žīąŽ≤ą-Žį§Ž≤ą)žôÄ ÍįôžĚÄ Žč§žĖĎŪēú Í∑ľŽ¨ī Žį©žč̞̥ ž†ĀÍ∑Ļž†ĀžúľŽ°ú ŽŹĄžěÖŪēī Ž≥ľ Í≤ɞ̥ Í∂ĆŪēúŽč§.
Žį§Ž≤ą Í∑ľŽ¨īžĚľžĚė Í≤Ĺžöį žĚľž£ľÍłįžú†ŪėēÍ≥ľ žÉĀÍīÄžóÜžĚī ŪŹČÍ∑† žąėŽ©īžčúÍįĄžĚī Ž™®ŽĎź 6žčúÍįĄ ŽĮłŽßĆžĚīžóąÍ≥†, 5žčúÍįĄ žĚīŪēėŽ°ú žąėŽ©īžĚĄ ž∑®ŪēėŽäĒ ŽĻĄžú®žĚī žĄł ÍĶį Ž™®ŽĎź 40%Ž•ľ ŽĄėŽäĒ Í≤ÉžúľŽ°ú ŽāėŪÉÄŽā¨Žč§. žĚīŽäĒ žĚľž£ľÍłįžú†Ūėēžóź ŽĒįŽ•ł Ž≤ĒŽ≤ą Í∑ľŽ¨īžĚľžĚė žąėŽ©īžčúÍįĄžĚī žį®žĚīÍįÄ žó܎觎äĒ žóįÍĶ¨[
27]žôÄ žú†žā¨Ūēú Í≤įÍ≥ľžĚīŽāė, žēĄžĻ®ŪėēžĚī Žį§Ž≤ą Í∑ľŽ¨īžĚľžĚė žąėŽ©īžčúÍįĄžĚī ž†ÄŽÖĀŪėēŽ≥īŽč§ ŽćĒ žßߎ觎äĒ Ž≥īÍ≥†[
11]žôÄŽäĒ Žč§Ž•ł Í≤įÍ≥ľžĚīŽč§. žĚīŽäĒ ŽĆÄžÉĀžěźžĚė Í∑ľŽ¨īŪėēŪÉúžĚė žį®žĚīžĚľ ÍįÄŽä•žĄĪžĚī žěąŽäĒŽćį žĄ†ŪĖČžóįÍĶ¨[
11]žĚė ŽĆÄžÉĀžěź ž§Ď 13.4%ŽßĆžĚī Ž≥ł žóįÍĶ¨ ŽĆÄžÉĀžěźž≤ėŽüľ ŽĻ†Ž•ł žąúŪôėÍĶźŽĆÄÍ∑ľŽ¨īŽ•ľ ŪēėÍ≥† žěąžóąŽč§. ž†ēžÉĀž†ĀžúľŽ°ú, ž†Ąž≤ī žĚľž£ľÍłį žčúžä§ŪÖú(circadian system)žĚī žě¨ž°įž†ēŽźėŽ†§Ž©ī Ž©įžĻ†žĚī žÜĆžöĒŽźėŽäĒŽćį[
29], ž£ľŽčĻ Ūēú Ž≤ą žĚīžÉĀ Í∑ľŽ¨īž°įÍįÄ ŽįĒŽÄĆŽäĒ ŽĻ†Ž•ł žąúŪôėÍĶźŽĆÄÍ∑ľŽ¨īŽ•ľ ŪēėŽäĒ Í≤Ĺžöį žÉĚž≤ī žĚľž£ľÍłį žčúžä§ŪÖú ž°įž†ēžóź žĖīŽ†§žõÄžĚī ŽćĒ ŽßéžĚĄ žąė žěąŽč§[
5]. Ž≥ł žóįÍĶ¨ ŽĆÄžÉĀžěźŽď§žĚė Žį§Ž≤ą Í∑ľŽ¨īŽäĒ 3žĚľ žĚīŽāīŽ°ú žßßžĚÄ ÍłįÍįĄžĚīŽĚľ ÍįúžĚłžĚė žĚľž£ľÍłįžú†ŪėēÍ≥ľ žÉĀÍīÄžóÜžĚī Ž™®Žď† ÍĶźŽĆÄÍ∑ľŽ¨īžěźÍįÄ žąėŽ©īžóź žĖīŽ†§žõĞ̥ Ž≥īžėĞ̥ ÍįÄŽä•žĄĪžĚī žěąŽč§. ŽėźŪēú Žį§Ž≤ą Í∑ľŽ¨ī žčú žąėŽ©īžčúÍįĄŽĆÄŽäĒ ŽĆÄŽ∂ÄŽ∂Ą Í∑ľŽ¨īŽ•ľ ŽßąžĻėÍ≥† 8žčúŽ∂ÄŪĄį žčúžěĎžĚī ŽźėŽäĒŽćį, Žį§ ŽŹôžēą Í∑ľŽ¨īŽ°ú žĚłŪēī Í≥ĄžÜć ÍĻ®žĖī žěąŽč§ÍįÄ Žāģžóź žąėŽ©īžĚĄ ž∑®ŪēėÍłį ŽēĆŽ¨łžóź žĚľž£ľÍłįŽ¶¨Žď¨žóź žĚėŪēú žąėŽ©īžĚī žēĄŽčĆ žąėŽ©īŽįēŪÉąžóź žĚėŪēú žąėŽ©īžĚī žßĄŪĖČŽźėŽäĒ Í≤ĹŪĖ•žĚī žěąžĖī[
30] ÍįúžĚłžĚė žĚľž£ľÍłįžú†Ūėēžóź žĚėŪēú žėĀŪĖ•žĚī ž†ĀžóąžĚĄ Í≤ÉžúľŽ°ú ž∂Ēž†ēŽźúŽč§. Í≤ĆŽč§ÍįÄ Žāģ žčúÍįĄžĚė žąėŽ©īžĚÄ žąėŽ©īžóź Ž∂Äž†ēž†Ā žėĀŪĖ•žĚĄ ž§Ą žąė žěąŽäĒ ŽĻõžĚīŽāė žÜĆžĚĆžóź ŽÖłž∂úŽźėÍłį žČ¨žöįŽĮÄŽ°ú[
17] žąėŽ©īžĚĄ ÍįúžĄ†ŪēėÍłį žúĄŪēīžĄúŽäĒ žēĒŽßČ žĽ§Ū侞̥ žā¨žö©ŪēėÍĪįŽāė žÜĆžĚƞ̥ ž§ĄžĚīÍłį žúĄŪēī Í∑ÄŽßąÍįúŽ•ľ žā¨žö©ŪēėŽäĒ ŽďĪžĚė ž†ĀÍ∑Ļž†ĀžĚł ŪôėÍ≤Ĺ ž°įž†ąžĚī ŪēĄžöĒŪē† Í≤ÉžĚīŽč§. Ž≥ł žóįÍĶ¨žóźžĄú ŽĻĄŽ°Ě žĚľž£ľÍłįžú†Ūėēžóź ŽĒįŽ•ł Žį§Ž≤ą Í∑ľŽ¨īžĚľžĚė žąėŽ©īžčúÍįĄžĚÄ žį®žĚīÍįÄ žóÜžßÄŽßĆ žā¨ŪöĆž†Ā žčúžį®žĚė žį®žĚīŽäĒ ÍįÄžě• žĽłŽč§. Žį§Ž≤ą Í∑ľŽ¨ī žčú žąėŽ©īžčúÍįĄžĚī Ūą¨žēĹ žė§Ž•ė ŽįúžÉĚÍ≥ľ ÍīÄŽ†® žěąžĚƞ̥ Í≥†Ž†§ŪēėŽ©ī[
7] ž†ĀÍ∑Ļž†ĀžĚł ž§Ďžě¨ÍįÄ ŪēĄžöĒŪēėŽč§. Žį§Ž≤ąžĚÄ žĚľž£ľÍłį žĶúž†Äž†ź(circadian nadir)žúľŽ°ú ÍįÄžě• ž°łŽ¶¨ŽäĒ žčúÍįĄŽĆĞ̳ 3žčúŽ∂ÄŪĄį 6žčú žā¨žĚīžóź Í∑ľŽ¨īŽ•ľ ŪēėÍłį ŽēĆŽ¨łžóź ÍĻ®žĖī žěąŽäĒŽćį žĖīŽ†§žõÄžĚī ŽßéŽč§[
5]. žēľÍįĄÍ∑ľŽ¨īžěźžĚė Í∑ľŽ¨ī ž§Ď žßßžĚÄ žąėŽ©ī(nap)žĚī Í∑ľŽ¨īžěźžĚė žĚłžßÄÍłįŽä•žóź ŽĮłžĻėŽäĒ žėĀŪĖ•žĚĄ ž°įžā¨Ūēú Ž©ĒŪÉÄŽ∂ĄžĄĚžóįÍĶ¨[
31]žóźžĄú 0žčúžóźžĄú 4žčú žā¨žĚīžóź 1žčúÍįĄ ŽĮłŽßĆžĚė žßßžĚÄ žąėŽ©īžĚĄ ž∑®ŪĖąžĚĄ ŽēĆ žąėŽ©ī ž†Ąžóź ŽĻĄŪēī ž†ĄŽįėž†Ā žĚłžßÄÍłįŽä•žĚī ž¶ĚžßĄŽźúŽč§Í≥† Ž≥īÍ≥†ŪēėžėÄŽč§. ŽĒįŽĚľžĄú žēľÍįĄÍ∑ľŽ¨ī ž§Ď žßßžĚÄ žąėŽ©īžĚĄ ž∑®Ūē† žąė žěąŽŹĄŽ°Ě ŪēėŽäĒ ž†ēžĪÖž†Ā ŽįįŽ†§ŽŹĄ Žį§Ž≤ąžĚė žąėŽ©īŽ∂Äž°ĪžĚĄ ÍįúžĄ†ŪēėŽäĒ Žćį ŽŹĄžõÄžĚī Žź† Í≤ÉžĚīŽč§.
ŪēúŪéł ŽāģŽ≤ąžĚīŽāė žīąŽ≤ą ŪõĄ ŪúīžĚľžóźžĄúŽäĒ žĚľž£ľÍłįžú†Ūėēžóź ŽĒįŽĚľ žąėŽ©īŽĻĄžú®žĚī ŽÜížĚÄ žčúÍįĄŽĆÄÍįÄ Žč§žÜĆ žį®žĚīÍįÄ žěąŽćĒŽĚľŽŹĄ žąėŽ©īžčúÍįĄŽĆÄÍįÄ žĚľž†ēŪēėÍ≤Ć ŪĆ®ŪĄīžĚī Ž≥īžĚīŽäĒ Í≤ÉÍ≥ľ Žč¨Ž¶¨, Žį§Ž≤ą ŪõĄ ŪúīžĚľžĚė žąėŽ©īžĚÄ Ž™®Žď† žĚľž£ľÍłįžú†ŪėēžóźžĄú žąėŽ©īžĚė Í∑úžĻôžĄĪžĚĄ žĄ§Ž™ÖŪēėÍłį žĖīŽ†§žõ†Žč§. žĚīŽäĒ Žį§Ž≤ą Í∑ľŽ¨ī ŪõĄ 2-3žĚľžĚė ŪúīžĚľ ŪõĄ Žč§žčú ŽāģŽ≤ąžĚīŽāė žīąŽ≤ąžúľŽ°ú Í∑ľŽ¨īž°įÍįÄ ŽįĒŽÄĆÍłį ŽēĆŽ¨łžóź žÉąŽ°úžöī Í∑ľŽ¨īž°įžóź ŽßěÍ≤Ć žąėŽ©īžčúÍįĄŽĆÄŽ•ľ žĚīŽŹôŪēėŽäĒ Í≥ľž†ēžóźžĄú ÍįúžĚłžĚė žÉĚž≤īžčúÍ≥ĄÍįÄ ž∂©Ž∂ĄŪěą žĚīŽŹôŪēėžßÄ Ž™ĽŪēīžĄú Žč§Ž•ł Í∑ľŽ¨īž°įžĚė ŪúīžĚľŽ≥īŽč§ Ūõ®žĒ¨ Ž∂ąÍ∑úžĻôŪēú žąėŽ©īžĚĄ Ž≥īžėĞ̥ Í≤ÉžúľŽ°ú ž∂Ēž†ēŽźúŽč§. Í∑ľŽ¨īž°į Ž≥ÄŪôĒžóź ŽĒįŽ•ł ŪöĆŽ≥ĶžčúÍįĄžĚī žßßžúľŽ©ī žąėŽ©īžóź žėĀŪĖ•žĚĄ ž§Ą žąė žěąžúľŽĮÄŽ°ú[
5], Žį§Ž≤ą Í∑ľŽ¨ī ŪõĄ ŪúīžĚľžĚÄ ŽāģŽ≤ąžĚīŽāė žīąŽ≤ąŽ≥īŽč§ŽäĒ ŽćĒ ÍłłÍ≤Ć Žįįž†ēŪē† ŪēĄžöĒÍįÄ žěąÍ≤†Žč§. 2018ŽÖĄ Ž≥ĎžõźÍįĄŪėłžā¨Ūöƞ󟞥ú ÍįĄŪėłžā¨ Í∑ľŽ¨īŪėēŪÉúŽ•ľ ž°įžā¨ŪĖąžĚĄ ŽēĆ ŽĆÄžÉĀ Ž≥ĎžõźžĚė 62%ÍįÄ žēľÍįĄž†ĄŽčīž†úŽ•ľ žčúŪĖČŪēėÍ≥† žěąŽč§Í≥† ŪēėžėÄŽäĒŽćį[
18], Ž≥ł žóįÍĶ¨Í≤įÍ≥ľžóźžĄú Ž≥īžĚł Í≤ÉÍ≥ľ ÍįôžĚī Žį§Ž≤ą Í∑ľŽ¨ī ŪõĄ ŪúīžĚľžĚė žąėŽ©ī ŪäĻžĄĪžĚĄ Í≥†Ž†§ŪēīžĄú ž∂©Ž∂ĄŪēú ŪúīžĚľ žąėÍįÄ Žįįž†ēŽź† žąė žěąŽŹĄŽ°Ě Ūēīžēľ Ūē† Í≤ÉžĚīŽč§.
Í∑ľŽ¨īž°įŽ≥Ą Í∑ľŽ¨īžĚľÍ≥ľ ŪúīžĚľ ÍįĄ žā¨ŪöĆž†Ā žčúžį®ŽäĒ Í∑ľŽ¨īžĚľÍ≥ľ ŪúīžĚľ ÍįĄ žąėŽ©īžčúÍįĄŽĆÄÍįÄ ÍłČÍ≤©ŪēėÍ≤Ć Ž≥ÄŪēėŽäĒ Žį§Ž≤ą Í∑ľŽ¨īž°įžĚľ ŽēĆ Ž™®Žď† žĚľž£ľÍłįžú†ŪėēžóźžĄú 5žčúÍįĄ žĚīžÉĀ Ž≤ĆžĖīžßÄŽäĒ Í≤ÉžúľŽ°ú ŪôēžĚłŽźėžóąŽäĒŽćį, ŪäĻŪěą žēĄžĻ®ŪėēÍĶįžĚī Žį§Ž≤ą Í∑ľŽ¨īŽ•ľ ŪēėŽäĒ Í≤Ĺžöį 7.37žčúÍįĄžúľŽ°ú ÍįÄžě• ŪĀį žčúžį®Ž•ľ Ž≥īžėÄŽč§. žú†ŽüŞ󟞥ú žčúŪĖČŪēú žÉĀÍ∑ľžěźžĚė žā¨ŪöĆž†Ā žčúžį® Ž∂ĄŪŹ¨Ž•ľ ž°įžā¨Ūēú žóįÍĶ¨[
13]žóź ŽĒįŽ•īŽ©ī, žčúžį®ÍįÄ žóÜŽäĒ Í≤ĹžöįÍįÄ 12.4%, 1žčúÍįĄ žĚīŪēėÍįÄ 38.8%, 1-2žčúÍįĄžĚī 29.1%Ž°ú ŽĆÄžÉĀžěźžĚė ŽĆÄŽ∂ÄŽ∂ĄžĚī 2žčúÍįĄ žĚīŪēėžĚė žā¨ŪöĆž†Ā žčúžį®Ž•ľ Ž≥īžėÄŽč§. žÉĀÍ∑ľžěźÍįÄ Ž≥īŪÜĶ ž£ľ 5žĚľž†ú Í∑ľŽ¨īŽ°ú žąėŽ©īžĚī Ž≥ÄŪēėŽäĒ Í≤Éžóź ŽĻĄŪēī, 3ÍĶźŽĆÄÍįĄŪėłžā¨ŽäĒ ÍĶźŽĆÄ ž£ľÍłįÍįÄ 5žĚľ ŽĮłŽßĆžúľŽ°ú Ž≥ÄŪēėŽäĒ Í≤ĹžöįÍįÄ ŽćĒ ŽßéÍ≥†[
17], žā¨ŪöĆž†Ā žčúžį®ŽŹĄ žÉĀÍ∑ľžěźŽ≥īŽč§ žĽ§žĄú ÍĪīÍįēžóź ŽĮłžĻėŽäĒ žėĀŪĖ•žĚī ŪĀī Í≤ÉžúľŽ°ú ž∂Ēž†ēŽźúŽč§. ŽĒįŽĚľžĄú žā¨ŪöĆž†Ā žčúžį®Ž•ľ ž§ĄžĚīÍłį žúĄŪēú ž†ĀÍ∑Ļž†ĀžĚł ŽÖłŽ†•žĚī ŪēĄžöĒŪēúŽćį, Ž≥ł žóįÍĶ¨žóźžĄú žīąŽ≤ąžĚÄ žā¨ŪöĆž†Ā žčúžį®ÍįÄ Ž™®Žď† ÍĶįžóźžĄú 1žčúÍįĄ ŽĮłŽßĆžúľŽ°ú ž†ĀžßÄŽßĆ, ŽāģŽ≤ąžóźžĄúŽäĒ ž†ÄŽÖĀŪėēžĚī, Žį§Ž≤ąžĚÄ žēĄžĻ®ŪėēžĚī žā¨ŪöĆž†Ā žčúžį®ÍįÄ žĽłžúľŽĮÄŽ°ú žĚľž£ľÍłįžú†ŪėēžĚĄ Í≥†Ž†§Ūēú Í∑ľŽ¨ī ž°įž†ēÍ≥ľ ÍįôžĚÄ Ž≥īŽč§ ž†ĀÍ∑Ļž†ĀžĚł ž§Ďžě¨ÍįÄ ŪēĄžöĒŪēėÍ≤†Žč§.
ž£ľÍīÄž†Ā žąėŽ©īžě•žē† ž†źžąėŽäĒ žĄł ÍĶįÍįĄ žú†žĚėŪēú žį®žĚīŽ•ľ Ž≥īžėÄžßÄŽßĆ, žā¨ŪõĄÍ≤Äž†ē Í≤įÍ≥ľžôÄ žąėŽ©īžě•žē† ŽĻąŽŹĄŽäĒ žú†žĚėŪēú žį®žĚīŽ•ľ Ž≥īžĚīžßÄ žēäžēėŽč§. ž†Ąž≤ī ŽĆÄžÉĀžěź ž§Ď 33.7%ÍįÄ ž£ľÍīÄž†Ā žąėŽ©īžě•žē†ÍįÄ žěąŽäĒ Í≤ÉžúľŽ°ú ž°įžā¨ŽźėžóąŽäĒŽćį žĚīŽäĒ 40žĄł žĚīžÉĀ žßÄžó≠žā¨ŪöĆ žĚłÍĶ¨Ž•ľ ŽĆÄžÉĀžúľŽ°ú ŽŹôžĚľŪēú ŽŹĄÍĶ¨Ž°ú žąėŽ©īžě•žē†Ž•ľ ž°įžā¨Ūēú žóįÍĶ¨[
32]žóźžĄú 9.26%Ž°ú Ž≥īÍ≥†Žźú Í≤ÉÍ≥ľ ŽĻĄÍĶźŪēėŽ©ī ŪėĄž†ÄŪěą ŽÜížĚÄ Í≤ɞ̥ žēĆ žąė žěąŽč§. žóįŽ†ĻžĚī ž¶ĚÍįÄŪē†žąėŽ°Ě žąėŽ©īžčúÍįĄžĚÄ ž§ĄÍ≥†[
26], žąėŽ©īžě•žē† ŽĻąŽŹĄŽäĒ ž¶ĚÍįÄŪēėŽäĒŽćį[
32], Ž≥ł žóįÍĶ¨ ŽĆÄžÉĀžěźŽď§žĚė žóįŽ†ĻžĚī žĄ†ŪĖČžóįÍĶ¨ ŽĆÄžÉĀžěźŽď§Ž≥īŽč§ ŽāģžĚƞ󟎏Ą žąėŽ©īžě•žē† ŽĻąŽŹĄÍįÄ ŽÜížēėŽćė Í≤ÉžĚÄ ÍĶźŽĆÄÍ∑ľŽ¨ī žěźž≤īÍįÄ ž£ľžöĒ žąėŽ©īžě•žē† žöĒžĚłžěĄžĚĄ žčúžā¨ŪēúŽč§.
Eastman [
33]žĚÄ ÍĶźŽĆÄÍ∑ľŽ¨ī žčú žĚľž£ľÍłįŽ¶¨Žď¨žĚī ÍĶźŽĆÄÍ∑ľŽ¨īžóź Žß쎏ĄŽ°Ě Ž≥ÄŪôĒŽźėÍłį žúĄŪēīžĄúŽäĒ žąėžčúŽ°ú Ž≥ÄŪēėŽäĒ ŽĻ†Ž•ł ÍĶźŽĆÄŽ≥īŽč§ŽäĒ ŽŹôžĚľŪēú Í∑ľŽ¨īž°įÍįÄ 1ž£ľ ž†ēŽŹĄ žú†žßÄŽźėŽäĒ ŽäźŽ¶į ÍĶźŽĆÄÍ∑ľŽ¨īŽ•ľ ž∂Ēž≤úŪēėÍ≥† žěąžúľŽ©į, Í∑ľŽ¨īŪėēŪÉúÍįÄ ŽįĒŽÄĒ ŽēĆŽäĒ ž†ĀžĖīŽŹĄ 2-3žĚľ žĚīžÉĀ ŪúīžĚľžĚĄ ž£ľŽŹĄŽ°Ě ž∂Ēž≤úŪēėÍ≥† žěąŽč§. ŽėźŪēú žĚľž£ľÍłįŽ¶¨Žď¨žĚī žěė Ž≥ÄŪôĒŪē† žąė žěąŽŹĄŽ°Ě ž†Āž†ąŪēú žčúÍįĄŽĆÄžóź ÍīĎ ŽÖłž∂úÍ≥ľ ÍīĎ ž†úŪēúžĚĄ Ž≥ĎŪĖČŪēėŽŹĄŽ°Ě Í∂ĆÍ≥†ŪēėÍ≥† žěąŽč§. Ž≥ł žóįÍĶ¨ ŽĆÄžÉĀÍ≥ľ ÍįôžĚī ŽĻ†Ž•ł žąúŪôėÍĶźŽĆÄÍ∑ľŽ¨īŽ•ľ ŪēėŽäĒ ÍįĄŪėłžā¨Žď§žóźÍ≤Ć Žį§Ž≤ą Í∑ľŽ¨ī ž†Ą 40Ž∂ĄÍįĄ ÍīĎ žĻėŽ£ĆŽ•ľ ŪēėÍ≥†, Í∑ľŽ¨īŽ•ľ ŽßąžĻú ŪõĄ žĄ†ÍłÄŽĚľžä§Ž•ľ žį©žö©Ūēī ŽĻõžĚĄ ž†úŪēúŪēėŽäĒ ž§Ďžě¨Ž•ľ ž†Āžö©Ūēú Í≤įÍ≥ľ, ÍįĄŪėłžā¨Žď§žĚė ŪĒľŽ°úŽŹĄÍįÄ ÍįźžÜĆŪēėÍ≥† žóÖŽ¨ī žė§Ž•ėÍįÄ ž§ĄžóąžúľŽ©į, ŪäĻŪěą ž†ÄŽÖĀŪėēžóźžĄú Í∑ł Ūö®Í≥ľÍįÄ ŽćĒ ÍįēŽ†•ŪēėŽč§Í≥† Ž≥īÍ≥†ŪēėžėÄŽč§[
34]. ŽĻĄŽ°Ě Ž≥ł žóįÍĶ¨žóźžĄú žĚľž£ľÍłįžú†Ūėēžóź ŽĒįŽ•ł ž£ľÍīÄž†Ā žąėŽ©īžě•žē† ŽĻąŽŹĄŽäĒ žį®žĚīÍįÄ žóÜžóąžßÄŽßĆ, žĚľž£ľÍłįžú†Ūėēžóź ŽĒįŽĚľ Í∑ľŽ¨īž°įŽ≥Ą žąėŽ©īžčúÍįĄžĚī Žč§Ž•ł Í≤ɞ̥ Í≥†Ž†§ŪēúŽč§Ž©ī, ÍĶźŽĆÄÍ∑ľŽ¨īžěźžĚė Í∑ľŽ¨īžĚľž†ēžĚĄ ž°įž†ēŪē† ŽēĆ ÍįúžĚłžĚė žĚľž£ľÍłįžú†Ūėēžóź Žßěž∂į Í∑ľŽ¨īŽ•ľ ŽįįžĻėŪē† ŪēĄžöĒÍįÄ žěąŽč§. žąėŽ©īžě•žē†Ž•ľ ŪėłžÜĆŪēėŽäĒ Í∑ľŽ°úžěźŽäĒ Í∑łŽ†ážßÄ žēäžĚÄ ÍĶįžóź ŽĻĄŪēī ž†ēžč† ÍĪīÍįēžĚĄ ŽĻĄŽ°ĮŪēú žó¨Žü¨ ÍĪīÍįē Ž¨łž†úŽ°ú žßĄŽ£Ć ŽėźŽäĒ žēĹŽ¨ľ ž≤ėŽį©Ž•†žĚī 2.8Žįį ŽÜíÍ≥†[
35], ÍĶźŽĆÄÍ∑ľŽ¨īŽäĒ ÍįĄŪėłžā¨žĚė ž£ľžöĒ žā¨žßĀ žöĒžĚł ž§Ď ŪēėŽāėžĚīŽč§[
36]. ŽĒįŽĚľžĄú ÍĶźŽĆÄÍ∑ľŽ¨ī ÍįĄŪėłžā¨žĚė Í≥†žö©žĚĄ žú†žßÄŪēėÍłį žúĄŪēīžĄúŽäĒ žąėŽ©īžĚĄ ÍįúžĄ†ŪēėÍłį žúĄŪēú Žč§žĖĎŪēėÍ≥† ž†ĀÍ∑Ļž†ĀžĚł ŽÖłŽ†•žĚī ŪēĄžöĒŪēėŽč§.
Ž≥ł žóįÍĶ¨žĚė ž†úŪēúž†źžĚÄ Žč§žĚĆÍ≥ľ ÍįôŽč§. Ž≥ł žóįÍĶ¨žóźžĄú ž°įžā¨Ūēú žąėŽ©īžčúÍįĄžĚÄ žąėŽ©īžĚľžßÄŽāė žē°ŪčįÍ∑łŽěėŪĒĄŽ°ú Í∑ľŽ¨īž°įŽ≥Ą Í∑ľŽ¨īžĚľÍ≥ľ ŪúīžĚľžĚė žąėŽ©īžčúÍįĄžĚĄ žł°ž†ēŪēėžßÄ žēäÍ≥† žĄ§Ž¨łžßÄŽ•ľ ŪÜĶŪēī ŪöĆžÉĀÍłįžĖĶžóź žĚėž°īŪēīžĄú ÍłįŽ°ĚŪēėžėÄÍłį ŽēĆŽ¨łžóź ÍįĚÍīÄžĄĪžĚī Žč§žÜĆ ŽĖ®žĖīžßą žąė žěąŽäĒ ž†úŪēúž†źžĚī žěąŽč§. Í∑łŽüľžóźŽŹĄ, Ž≥ł žóįÍĶ¨ŽäĒ Í∑ľŽ¨īž°įŽ≥Ą žąėŽ©īžĚĄ ž°įžā¨Ūēėžó¨ žĚľž£ľÍłįžú†ŪėēÍ≥ľ žąėŽ©īžĚė ÍīÄŽ†®žĄĪžĚĄ ž°įžā¨Ūēú žóįÍĶ¨Ž°ú, ÍĶźŽĆÄÍ∑ľŽ¨īÍįĄŪėłžā¨žóźÍ≤Ć Ž≥īŽč§ ž†ĀŪē©Ūēú Í∑ľŽ¨īžú†ŪėēžĚĄ ÍįúŽįúŪēėÍ≥† ž†Āžö©ŪēėŽäĒŽćį ÍłįžīąÍįÄ ŽźėŽäĒ žěźŽ£ĆŽ°úžĄú žĚėžĚėÍįÄ žěąŽč§.



 PDF Links
PDF Links PubReader
PubReader Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print